|
|
||||||||||||||||||||||||||||||||||||
Disease Conditions
- Abscess
- Acne
- Addiction
- Adenoid Hypertrophy
- Allergic Rhinitis or Hay Fever
- Alopecia Areata
- Alzheimers Disease
- Amoebiasis
- Anxiety
- Asthma
- Backache
- Bed-Wetting-Enuresis
- Brain-Tumour
- Cataract
- Cirrhosis of Liver
- Conjunctivitis
- Constipation
- Dengue
- Depression
- Diabetes Mellitus
- Diseases of Prostate
- Eczema
- Epilepsy
- Erectile-Dysfunction
- Gallstones
- Goitre
- Gynaec
- Hepatitis
- Hepatitis-a
- Hepatitis-b
- Hepatitis-e
- Hyperthyroidism
- Hypothyroidism
- IBS - Irritable Bowel Syndrome
- Infertility
- Infertility FAQ
- Male Infertility
- Male Infertility FAQ
- Women Infertility
- Lichen Planus
- Lipoma
- Meningitis
- Menstrual-Disorders
- Migraine
- Molluscum-Contagiosum
- Nasal-Polyps
- Neoplasm
- Nephrotic Syndrome
- Neuralgia
- Osteo Arthritis
- Otitis
- Piles or Hemorrhoids
- Premature-Ejaculation
- Psoriasis
- Rheumatoid Arthritis
- Ringworm
- Schizophrenia
- Sinusitis
- Spondylitis
- Styes
- Tarsal Cyst-Chalazion
- Tonsilitis
- Typhoid
- Urinary-Tract-Infection
- Urticaria
- Vertigo
- Vitiligo
- Warts
Auroh Health Horoscope
Disease A - Z > Bed Wetting Enuresis > Homeopathic treatment for Bed Wetting Enuresis
Homeopathy treatment for Bed Wetting Enuresis
|
||||||||
What is Bed-Wetting/Enuresis ?
Bed-wetting is urination during sleep. Children learn bladder control at different ages. Children younger than 4 often wet their bed or clothes because they can't yet control their bladder. But most children can stay dry through the night by age 5 or 6.
Bed-wetting is defined as a child age 5 or older wetting the bed at least 1 or 2 times a week over at least 3 months. In some cases, the child has been wetting the bed all along. But bed-wetting can also start after a child has been dry at night for a long time.
Wetting the bed can be upsetting, especially for an older child. Your child may feel bad and be embarrassed. You can help by being loving and supportive. Try not to get upset or punish your child for wetting the bed.
There is also the problem of cleaning the soiled mattress or finding a quality mattress protector. Alternatively, you may have to buy a new mattress altogether. You can find great deals for all your mattress needs by shopping for a mattress at 1800mattress.com or other discount online retailers.
The age at which bladder control is expected varies considerably.
- Some parents expect dryness at a very early age, while others not until much later. Such a time line may reflect the culture and attitudes of the parents and caregivers.
- Factors that affect the age at which wetting is considered a problem include the following:
- The child's gender: Bedwetting is more common in boys.
- The child's development and maturity
- The child's overall physical and emotional health -- chronic illness and/or emotional and physical abuse may predispose to bedwetting.
Bedwetting is a very common problem.
- Parents must realize that enuresis is involuntary. The child who wets the bed needs parental support and reassurance.
- About 5-7 million children in the United States wet the bed. Most children simply outgrow bedwetting with a rate of resolution of the issue of about 15% per year.
- The prevalence of childhood primary enuresis (see below for definition) is:
- 5 years old 16%
- 6 years old 13%
- 7 years old 10%
- 8 years old 7%
- 10 years old 5%
- 12-14 years old 2%-3%
- over 15 years old 1%-2%
Bedwetting is a treatable condition.
- While children with this embarrassing problem and their parents once had few choices except waiting to "grow out of it," there are now treatments that work for many children.
- Several devices, treatments, and techniques have been developed to help these children stay dry at night.
Types of bedwetting
Two types of bedwetting occur:
- Primary enuresis -- bedwetting since infancy; and
- Secondary enuresis -- wetting developed after being continually dry for a minimum of six months.
What is primary bedwetting ?
Primary bedwetting is generally viewed as a delay in maturation of the nervous system. At 5 years of age, approximately 20% of children wet the bed at least once a month with about 5% of males and 1% of females wetting nightly. By 6 years of age, only about 10% of children are bedwetters -- the large majority being boys. The percentage of all children who are bedwetters continues to diminish by 50% each year after 5 years of age. Family history plays a big roll in predicting primary bedwetting. If one parent was a bedwetter, the offspring have a 45% chance of a developing primary enuresis as well.
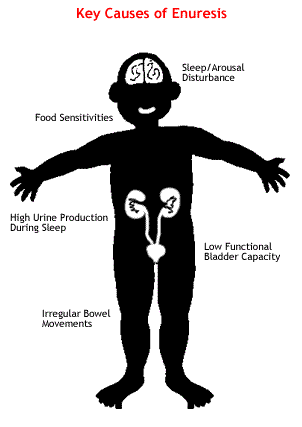 |
What causes secondary bedwetting ?
Urinary tract infections, metabolic disorders (for example, various types of diabetes), external pressure on the bladder (for example, extreme constipation by a large rectal stool mass), as well as neurologic disorders of the spinal cord must be considered among the causes of secondary bedwetting.
How is the cause of secondary bedwetting diagnosed ?
Generally, a complete history and thorough physical exam provide the initial evaluation of a child with primary bedwetting. A urinalysis and urine culture generally complete the workup. Further laboratory and radiological studies are usually reserved for the youngster who presents with secondary bedwetting.
Self-Care at Home
Here are some tips for helping your child stop wetting the bed. These are techniques that are most often successful.
- Reduce evening fluid intake. The child should try to not take excessive fluids, chocolate, caffeine, carbonated drinks, or citrus after 3 p.m. Routine fluids with dinner are appropriate.
- The child should urinate in the toilet before bedtime.
- Set a goal for the child of getting up at night to use the toilet. Instead of focusing on making it through the night dry, help the child understand that it is more important to wake up every night to use the toilet.
- A system of sticker charts and rewards works for some children. The child gets a sticker on the chart for every night of remaining dry. Collecting a certain number of stickers earns a reward. For younger children, such a motivational approach has been shown to provide significant improvement (14 consecutive dry nights) in approximately 70% of children with a relapse rate (two wet nights out of 14) of only 5%.
- Make sure the child has safe and easy access to the toilet. Clear the path from his or her bed to the toilet and install night-lights. Provide a portable toilet if necessary.
- Some believe that you should avoid using diapers or pull-ups at home because they can interfere with the motivation to wake up and use the toilet. Others argue that pull-ups help the child feel more independent and confident. Many parents limit their use to camping trips or sleepovers.
The parents' attitude toward the bedwetting is all-important in motivating the child.
- Focus on the problem: bedwetting. Avoid blaming or punishing the child. The child cannot control the bedwetting, and blaming and punishing just make the problem worse.
- Be patient and supportive. Reassure and encourage the child often. Do not make an issue out the bedwetting each time it happens.
- Enforce a "no teasing" rule in the family. No one is allowed to tease the child about the bedwetting, including those outside the immediate family. Do not discuss the bedwetting in front of other family members.
- Help the child understand that the responsibility for being dry is his or hers and not that of the parents. Reassure the child that you want to help him or her overcome the problem. If applicable, remind him that a close relative successfully dealt with this same issue.
- The child should be included in the clean-up process.
To increase comfort and reduce damage, use washable absorbent sheets, waterproof bed covers, and room deodorizers.
Self-awakening programs are designed for children who are capable of getting up at night to use the toilet, but do not seem to understand its importance.
- One technique is to have the child rehearse the sequence of events involved in getting up from bed to use the toilet during the night prior to going to bed each night.
- Another strategy is daytime rehearsal. When the child feels the urge to urinate, he or she should go to bed and pretend he or she is sleeping. He or she should then wait a few minutes and get out of bed to use the toilet.
Parent-awakening programs can be used if self-awakening programs fail. These programs should only be used at the child's request.
- The parent should awaken the child, typically at the parents' bedtime.
- The child must then locate the bathroom on his or her own for this to be productive. The child needs to be gradually conditioned to awaken easily with sound only.
- When this is done for seven nights in a row, the child is either cured or ready for self-awakening programs or alarms.
Bedwetting alarms have become the mainstay of treatment.
- Up to 70% of children stop bedwetting after using these alarms for 12-16 weeks.
- About 20%-30% start wetting the bed again when the alarm is discontinued (relapse). However, the positive response to reinstating the alarm system is rapid due to the behavioral conditioning experienced during the first treatment cycle. With persistence, this method works for 50%-70% in the long run.
- These alarms take time to work. The child should use the alarm for a few weeks or even months before considering it a failure.
- There are two types of alarms: audio and tactile (buzzing) alarms.
- The principle is that the wetness of the urine bridges a gap in the sensor, which in turn sets off the alarm. The sensor is placed either on the child's underwear or bed pad.
- The child then awakens, shuts off the alarm, finishes urinating in the toilet, returns to the bedroom, changes clothes and the bedding, wipes down the sensor, resets the alarm, and returns to sleep.
- Alarms are preferred over medications for children because they have no side effects.
- It is generally believed that all children 7 years and older should be given a trial of an alarm.
- For the alarm to be effective, the child must desire to use it. Both the child and parents need to be highly motivated.
Auroh Homeopathic Treatment For Bedwetting
As most of the primary bedwetters have a problem of nervous system, homeopathic medicines help regulating the system and help alleviate the problem of bedwetting.
Homeopathic remedies play a vital role in treating infection of urinary bladder or kidneys, hence relieving the problem completely.
Auroh Homeopathic medicines offer excellent relief for Bedwetting. Homeopathic medications can relieve the incontinency and stimulate the nervous system without any side effects and is good for raising the immunity. homeopathy is of use in eradicating chronic relapsing conditions. Homoeopathy doesnt treat the disease in man but it treats the man in disease. Homoeopathy treats the cause of disease and the illness will disappear.
homeopathy is strongly recommended in cases of Bedwetting
| talk to our doctors right now |  |
|
| consult our experts | ||
 |
leave your number we will call you back |
|
| start auroh health treatment |
Your doctor is just a click away |
Treatment |